
By Bill Hammond
Courtesy of The Empire Center
As Washington threatens to crack down on fraud and abuse in New York’s Medicaid program, state legislators are doing their best to demonstrate why federal intervention is needed.
A glitch in the state’s “surprise billing” law is allowing certain physicians to extract Medicaid fees that are sometimes hundreds of times higher than the safety-net health plan normally pays – a maneuver that’s costing state taxpayers an estimated $56 million annually.
For the second year in a row, Governor Hochul’s budget plan called for shutting down this rapidly growing loophole and, for the second in a row, Assembly and Senate leaders dropped her fix from their respective one-house budgets without offering a better solution of their own.
Unless Hochul changes their minds, an egregious racket against taxpayers is likely to keep getting worse.
At issue is a law passed in 2014 that’s meant to shield consumers from so-called surprise bills when they receive emergency treatment by doctors and hospitals outside their insurance plan’s coverage network.
Under this law, out-of-network emergency providers can no longer bill patients for amounts not covered by insurance. Instead, dissatisfied providers can seek more money from insurers through an arbitration process known as independent dispute resolution, or IDR.
Arbitrators involved in IDR are supposed to base their decisions on the 80th percentile of relevant fees paid by commercial insurers in each region of the state, as determined by a claims tracking organization known as Fair Health.
IDR was not expected to have any effect on Medicaid, because the program’s recipients are generally exempt from cost-sharing and therefore not vulnerable to surprise billing. However, the law does not explicitly exempt Medicaid, and a rapidly growing number of providers are using IDR to win payments that are dramatically higher. This is because the system uses commercial fees as its benchmark, whereas Medicaid – as a taxpayer-funded safety-net plan – has traditionally paid lower fees than private insurance.
In one real-life example cited in budget testimony by the New York Health Plan Association, an insurer ordered to pay $514,000 for emergency back surgery, which was 182 times the standard Medicaid fee of $2,807.
The Department of Financial Services says the number of IDR cases filed against insurers has soared by more than 600 percent in four years, from 2,500 in 2020 to 17,800 in 2024.
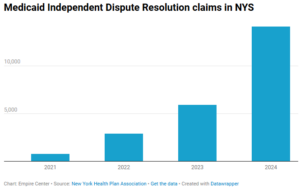
Data from the Health Plan Association suggest that the bulk of that increase was driven by Medicaid claims, which went from 778 in 2021 to 14,116 in 2024, an increase of more than 1,700 percent in three years.
Officials say New York’s IDR cases are concentrated on Long Island – and many are being brought through companies that file claims on behalf of providers in return for a percentage of the proceeds. One company, Callagy Recovery Corp., claims on its website that it has won 90 percent of its arbitration cases, boosted fees by an average of 980 percent and returned $1.3 billion to clients.
One of Callagy’s ads on Instagram showed a man in hospital scrubs and sunglasses standing in front of a sports car under the slogan: “Surgeons: It’s time to get paid what you deserve.”
Critics say the system has created an incentive for certain types of specialists – such as emergency room doctors and orthopedic surgeons – to refuse to join the provider networks of insurance plans and then systematically challenge all reimbursements through IDR.
A lawsuit recently filed by Fidelis, the state’s largest Medicaid managed care plans, describes a variation on that scheme: According to court papers, a Long Island-based practice called Centurion Brooklyn Anesthesiology agreed to be part of Fidelis’ provider network. But when its doctors provided treatment to Fidelis members, it submitted claims through a second company – Sedation Vacation Perioperative Medicine – which is registered at the same address with the same owner.
This second company claimed not to be part of the Fidelis network, enabling it to dispute its fees through IDR.
In response to these schemes, one of Hochul’s budget bills includes a set of changes to the surprise billing law – including one that would flatly exempt Medicaid claims from dispute resolution.
“We do not believe that the Medicaid program should be price-gouged by specialists, which is what is occurring with the IDR process,” state Medicaid Director Amir Bassiri said at February’s hearing on the health-care portions of the state budget.
Another of the governor’s proposed amendments would tighten IDR standards for private insurers, setting the 50th percentile of commercial claims as the benchmark for arbitration and the 80th percentile as a ceiling for payouts.
A third change would put the Empire Plan, which provides health benefits for state workers, under the jurisdiction of the updated state surprise-billing law instead of its federal counterpart.
These proposals, contained in Part T of the governor’s Public Protection and General Government budget bill, were entirely omitted from the budget counterproposals of both the Assembly and Senate.
This move apparently reflects concern some doctors, if denied IDR, would refuse to accept Medicaid at all – which would compromise care provided to Medicaid recipients.
Exempting Medicaid “is going to limit Black and brown communities from having access to specialists,” Assemblywoman Michelle Solages of Nassau County said at the health budget hearing.
It’s true that Medicaid typically pays lower fees to providers, especially physicians, and that this long-standing practice makes it harder for recipients to get appointments with specialists.
However, allowing a fraction of those specialists to extract exorbitant fees by gaming the legal system is the wrong way to address a systemic problem.
If the Legislature uses that concern as an excuse to reject Hochul’s simple reform – and turns a blind eye to blatant abuse – they will be confirming Washington’s worst fears about Albany and Medicaid fraud.
Bill Hammond is the Empire Center’s senior fellow for health policy.

